This post is also available in: 简体中文 繁體中文
OTTAWA—Now that Canada has an expanding menu of COVID-19 vaccines, you’re probably hearing chatter about how this one is better and that one is worse.
Dr. Alan Bernstein has this advice for you: take the first shot you can.
That’s what he’s going to do.
“All the vaccines are working really well — that’s the bottom line,” said Bernstein, the president of the research organization CIFAR and member of the federal government’s COVID-19 vaccine task force.
“I will take the first vaccine I’m offered,” he said.
It’s a message that health officials are trumpeting after Health Canada authorized the country’s fourth COVID vaccine last week, deeming the Johnson & Johnson shot safe and effective against the deadly coronavirus. Yes, each shot comes with a different “efficacy” rate — but that doesn’t mean you can easily conclude one is better than others.
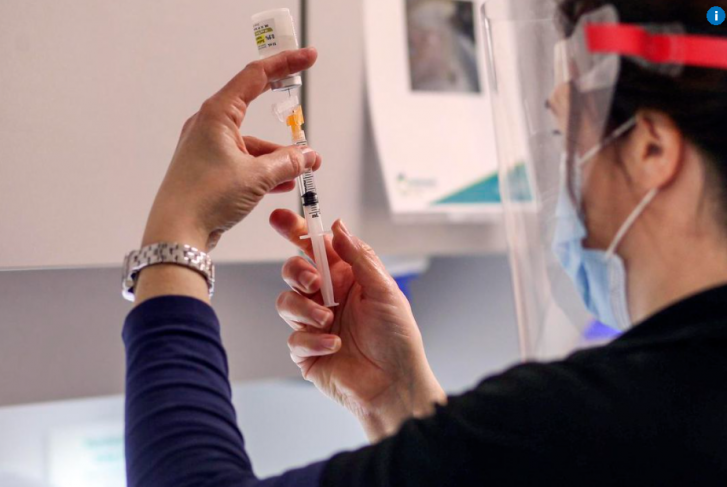
“I just wanted to caution against this sort of ‘good or bad vaccines,’” Dr. Supriya Sharma, Health Canada’s chief medical adviser, told reporters recently. “If there’s a vaccine and it’s been authorized by Health Canada, it means that it’s met standards.”
What, then, to make of the efficacy rates? At first blush, they seem significantly different. Health Canada concluded the Johnson & Johnson shot had a 66-per-cent efficacy. AstraZeneca’s vaccine had a rate of 62-per-cent, according to one set of data, while the first shots approved in Canada — those from Pfizer-BioNTech and Moderna — had efficacy rates higher than 90 per cent.
You might conclude the shots with higher efficacy rates are better at preventing COVID-19.
Not so fast, Bernstein said.
The first thing to know is that efficacy rates only reflect the result of a clinical trial. All that it indicates is the difference between the number of people in the placebo group and the group that got the vaccine who, for example, got COVID, Bernstein explained.
In other words, the number is an indication of how less likely you would be to get infected if you get the vaccine.
But that’s only based on the snapshot of a clinical trial, Bernstein said — a test on certain groups of people in certain areas at a certain point in time. The effectiveness of a vaccine in the “real world” will be different, and likely lower, Bernstein said.
“The people in the trial tend to be people in good health, whereas people in real life, people have cancer and heart disease and diabetes — all the things we know can suppress your immune response,” Bernstein said.
It’s better, then, to think of the efficacy rate as an initial “estimate” rather than a rock-solid fact about how effective a vaccine is against the virus, and that more information about the strength of defence they provide will emerge as more people get their shots, said Dr. Bradly Wouters, executive vice president of science at research at the University Health Network in Toronto.
Like Bernstein, Wouters said a range of factors from a clinical trial will affect the efficacy rate of the vaccines. One big one is where the trial took place, he said, pointing to how the Johnson & Johnson shot was tested in South Africa, where a mutation of the coronavirus emerged that is thought to be more contagious and resistant to the protective effects of the vaccines.
Each clinical trial also measures a different “end-point” for efficacy, whether it is preventing any COVID infection or preventing a certain level of severity, Bernstein said.
Such differences make it impossible to compare the vaccines based on efficacy rates from their clinical trials—a true case of “apples to oranges,” he said.
The bottom line for both experts is that all clinical trials showed each of the vaccines authorized in Canada protect against the most severe cases of COVID. As Wouters pointed out, none of the people who got a shot in any of the trials died from COVID.
In the battle against the virus, Wouters said, the most important thing is to get that protection from danger and to help the collective push for herd immunity by using the vaccines to reduce your chance of getting the virus — which will happen regardless of its efficacy rate in clinical trials.
“Getting as much vaccine to as many people as quickly as possible, we can reach that magic herd immunity number — it means that COVID will be driven away,” Wouters said.
In other words, follow Bernstein’s advice and take the first shot you can.
Article Source: The Star
Author: Alex Ballingall

