When the World Health Organization declared COVID-19 a pandemic, people were forced to think of alternative ways to provide in-person services to help slow the spread of infection.
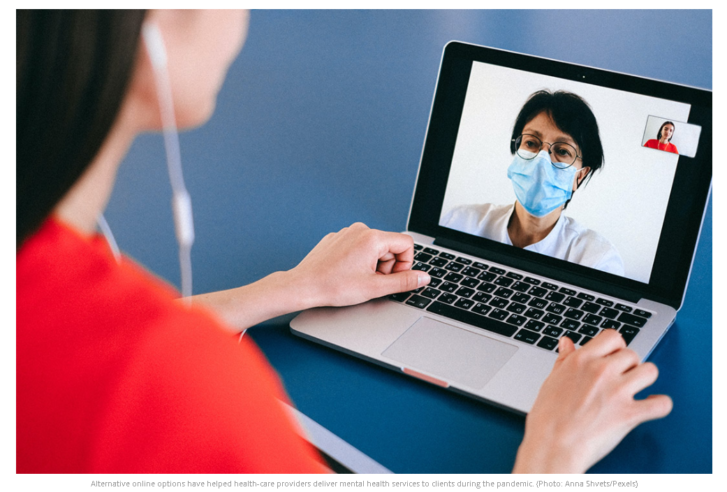
During a time when health-care professionals could no longer see patients in person, how did providers deliver mental health services to clients? The answer? Telehealth.
Telehealth uses both audio and video communication to deliver health care where providers and patients cannot be in the same room. When applied to mental health, this method is known as telepsychiatry. Although the use of telepsychiatry is not new, it was greatly underused prior to the pandemic.
“When health-care providers turned to telepsychiatry in place of face-to-face service delivery, the impact it would have on those with mental health conditions was unknown,” said University of Saskatchewan (USask) College of Nursing assistant professor Dr. Hua Li (PhD). “But mental health care is vital to manage symptoms for patients, so accessing services in one way or another was critical during the pandemic.”
Drs. Li, Arlene Kent-Wilkinson (PhD), Tracie Risling (PhD), and Don Leidl (EdD) from the USask College of Nursing, and Manal Kleib (PhD) from the University of Alberta Faculty of Nursing, were interested in whether the transition of mental health services to telepsychiatry during the pandemic was effective, especially from the perspectives of both service users and providers, and began a literature review to find the answer.
The research team found that, for the most part, the transition of mental health service delivery from face-to-face to telepsychiatry met or exceeded the expectations of patients and health-care providers.
“At the start of the pandemic during the rapid transition to telepsychiatry, there was an increase in people missing scheduled appointments, but within a few weeks and after the initial dip, people accepted the technology and the number of scheduled appointments went up and no-shows declined,” said Li.
Video consultation was the most popular form of telepsychiatry, followed by phone calls. Age was a strong contributing factor influencing which option was utilized, with those over 45 years of age choosing telephone visits and those under 45 choosing video.
Like all new forms of technology, there were advantages and disadvantages with the transition. Telepsychiatry increased access to mental health services, especially where there were geographic and financial barriers. Some patients found telepsychiatry to be less intimidating and thought their health-care providers made good decisions on treatment plans during virtual consults, while others found the virtual interaction to be impersonal and rushed.
Social determinants of health also played a key role in the acceptance of telepsychiatry during the pandemic. Not everyone can afford digital connectivity. Where the phone was used instead of video, health-care providers questioned the accuracy of their assessments when they couldn’t observe body language, behaviour and non-verbal cues, especially when diagnosing and treating new patients.
As the United Nations prepares to spotlight World Mental Health Day on Oct. 10, the successful growth of telehealth and telepsychiatry during the pandemic is providing another useful tool in the health care toolkit.
“The study findings showed that some patients and health-care providers would like to use telepsychiatry after the pandemic is over, while others prefer to go back to in-person services, in particular those over 45 years of age,” said Li.
The pandemic drastically sped up the adoption of telehealth visits and showed the health care world what technology can offer. Although most patients and health-care providers in the studies were comfortable with the transition and pleased with overall results, Drs. Li, Kent-Wilkinson, Risling, Leidl and Kleib found the recommendation to use a hybrid model between in-person appointments and telepsychiatry services would be best to meet the various needs among patients and providers in the post-pandemic years ahead.
Article From: University of Saskatchewan
Author: KYLIE KELSO

